|
www.HealthyHearing.com |
What to expect at a hearing test
By Joy Victory, managing editor, Healthy Hearing  Reviewed by
Megan Gerhart, audiologist Reviewed by
Megan Gerhart, audiologist Last updated on: December 19th, 2025 Hearing tests are used to detect and diagnose hearing loss. They are painless and noninvasive. Key points:
While often dismissed as not a big deal, hearing loss has far-reaching effects on your health. Getting a baseline hearing test and annual follow-up tests can help you catch it early and get the correct kind of hearing aids and levels of amplification to ensure you're hearing your best. What to expect during a hearing testYou can expect a hearing test to take about an hour. Here's what the process typically involves, and other important things to know:
1. Gathering your hearing health historyAt your first hearing clinic visit, you’ll fill out a case history form that helps your hearing care professional understand your medical and hearing health history. There are many potential causes of hearing loss, so the case history helps determine if you could have anything inherited or genetic in your family. Additionally, your hearing care provider may ask about non-inherited conditions that may contribute to hearing loss including:
They will also likely ask you about your work, hobbies, level of noise exposure, and what symptoms brought you in for your evaluation. 2. Pure-tone audiometryThe next part of a hearing test usually involves pure-tone audiometry, which includes listening to tones at different pitches and volumes. It occurs in a sound-treated room. Your hearing care professional will communicate with you and provide instructions through your headphones. You will have to focus and listen carefully because you need to respond even if the tone sounds very soft and you can barely hear it. The test measures the very softest sounds you can hear at each frequency tested. 3. Speech audiometrySpeech audiometry uses recorded or live speech instead of pure tones, in a quiet setting. The speech exam evaluates the softest speech sounds (threshold) you can hear and understand. You will then be asked to repeat back words that are presented at a level well above threshold to see how well you can understand them accurately. Some practitioners use speech sounds to determine your most comfortable listening level and the upper limits of comfort for listening. 4. 'Speech in noise' testsMost people complain about how they hear in noisy environments—not quiet sound-treated rooms. Common tests to replicate and quantify this hearing ability include the:
You may take one or more of these tests, depending on what your hearing specialist thinks is best. During these tests you will listen to a speaker say words and statements while a soundtrack plays increasingly noisy sounds. They are useful for assessing “real-world” hearing ability, mimicking how you might hear in a restaurant or noisy grocery store. This information will help your hearing care professional understand what technology will work best for you. After you receive your hearing aids, you may take a similar test to fine-tune the amplification levels on your aid. This is known as the hearing aid fitting. 5. Bone conduction testingIn some cases, a bone conduction test will also be given, which can help determine if the hearing loss is conductive or sensorineural. Treatment is generally different for people with conductive hearing loss. 6. Tympanometry and ear drum examTo check for ear wax blockage or other anatomical problems, your hearing care provider will use a device to look at your ear drum up close (see image). If necessary, your audiologist may perform tympanometry and a test of your acoustic reflexes. For these tests, a soft plug that creates pressure changes and generates sounds will be placed in the ear. This will determine how well your eardrum is moving and will measure the reflexive responses of the middle ear muscles. 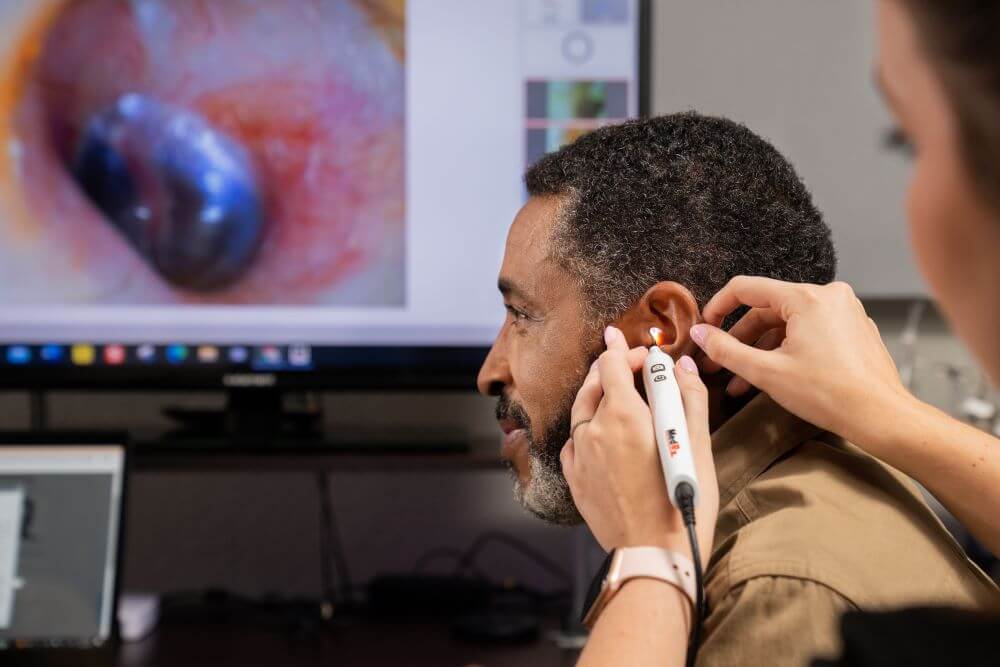
Frequently asked questions about hearing testsAre hearing tests painful?Not at all! Unlike a lot of medical tests, hearing tests are painless and non-invasive. Most occur in a quiet, sound-treated room (booth) or enclosure designed to keep out any other noises which might affect your hearing exam scores, such as the heater, air conditioner or office environment. You will be asked to wear headphones or soft earplugs with wires connected to an instrument called an audiometer that is used to conduct the test. Will I get my results right away?
Yes. Your hearing care provider will discuss your results with you right after testing is over. Test results are presented on a graph called an audiogram that displays the softest sounds you can hear at different pitches or frequencies. The vertical axis of an audiogram represents the intensity or volume of the sounds (in decibels, of dB). The horizontal axis depicts the frequency or pitch of the sound (in hertz, Hz). For each tone you heard during the test, there will be a mark on the audiogram at the appropriate decibel level. Each ear is plotted separately and represented by two different lines. The lines may be quite similar and follow the same pattern or they may be very different. 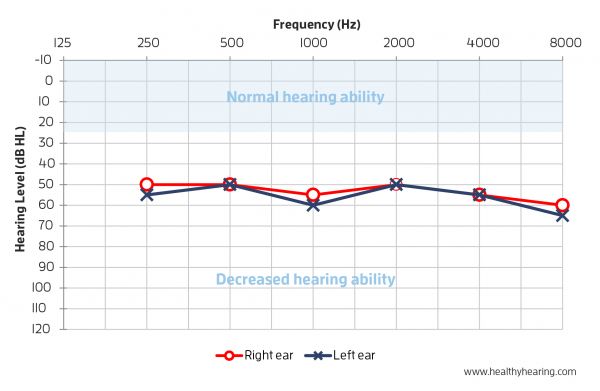
different pitches (frequencies). How do I know if my hearing is bad?Your hearing care provider will help you understand the severity of your hearing loss. Degrees of hearing loss is measured in decibels (dB) and in the following categories:
Although some people talk about hearing loss in terms of percentage, it is not an appropriate or meaningful measure of hearing loss. It is very common to have more hearing loss at some frequencies than for others, so the percentage of hearing loss would be different at each test frequency, making it virtually meaningless when describing the overall hearing loss or determining a course of treatment. Are online hearing tests reliable?It depends. There are a wide variety of hearing tests available online. Some are quiz-based screening tests (like ours), which can help you determine if you should go in for more rigorous in-person testing to determine the precise extent of your hearing loss. Some sites also have noise-based tests that let you listen to audio samples. While online hearing tests or the "Take a Hearing Test" for Apple AirPods Pro 3 can provide people with a snapshot of their hearing status, they are by no means a replacement for a thorough diagnostic hearing evaluation by a hearing professional. What if tests are normal, but I still struggle to hear?Some people have hearing loss that originates in their brain, and not their ears. This is known as hidden hearing loss. Standard hearing tests can't detect hidden hearing loss. If you passed your hearing test, but still feel like you can't hear well, you may have hidden hearing loss. How do I know if I'm a candidate for hearing aids?Once your testing is complete, if you have hearing loss, your hearing care professional will recommend treatment, which may include hearing aids, or other devices. Treating hearing loss is important for your communication ability, relationships, and overall health. If you’re ready to take the next step, find a trusted hearing care provider near you to get started. Our national directory includes thousands of consumer-reviewed hearing clinics. Joy Victory, managing editor, Healthy Hearing
You are reading about: Related topics
More information about hearing aids, hearing aid brands, assistive devices and tinnitus. Featured clinics near me
Earzlink Hearing Care - Reynoldsburg
HearingLife - Pickerington Find a clinicWe have more hearing clinic reviews than any other site! Related contentThe Healthy Hearing Report |
|
www.HealthyHearing.com |
What to expect at a hearing test
By Joy Victory, managing editor, Healthy Hearing  Reviewed by
Megan Gerhart, audiologist Reviewed by
Megan Gerhart, audiologist Last updated on: December 19th, 2025 Hearing tests are used to detect and diagnose hearing loss. They are painless and noninvasive. |




 Joy Victory has extensive experience editing consumer health information. Her training in particular has focused on how to best communicate evidence-based medical guidelines and clinical trial results to the public. She strives to make health content accurate, accessible and engaging to the public.
Joy Victory has extensive experience editing consumer health information. Her training in particular has focused on how to best communicate evidence-based medical guidelines and clinical trial results to the public. She strives to make health content accurate, accessible and engaging to the public.