|
www.HealthyHearing.com |
Hearing loss tests
By Joy Victory, managing editor, Healthy Hearing Last updated on: September 3rd, 2024 A thorough hearing test is easy and painless, and it will get you started on your path to better hearing. Find out what to expect when you are tested for hearing loss. Although we don't tend to think of it this way, hearing loss is highly unique—some people can't hear high-pitched sounds while others can't hear low-pitched sounds, for example. In many cases, hearing loss also progresses so gradually that it can be difficult to notice. While often dismissed as not a big deal, this is a myth. Hearing loss has far-reaching effects on your health. Getting a baseline hearing test and annual follow-up tests can help you catch it early and get the correct kind of hearing aid and levels of amplification to ensure you're hearing your best. A thorough hearing test can also help define the type of hearing loss you have: conductive, sensorineural or mixed and whether it will respond best to medical treatment, hearing aids, bone-anchored hearing systems or cochlear implants. Do you need a hearing test?Regardless of your age or job, you should get a hearing test if you (or a loved one) feel like you're not hearing as well as you used to. Those most at risk of hearing loss are people older than 60, and workers in high-noise occupations, such as construction or restaurants. Here's how to know if you need your hearing tested. If you've already confirmed you have hearing loss through testing, then you should speak to your hearing care practitioner about how often you should get re-tested. Much like vision, hearing can change over time, and hearing aids also need periodic adjustments. 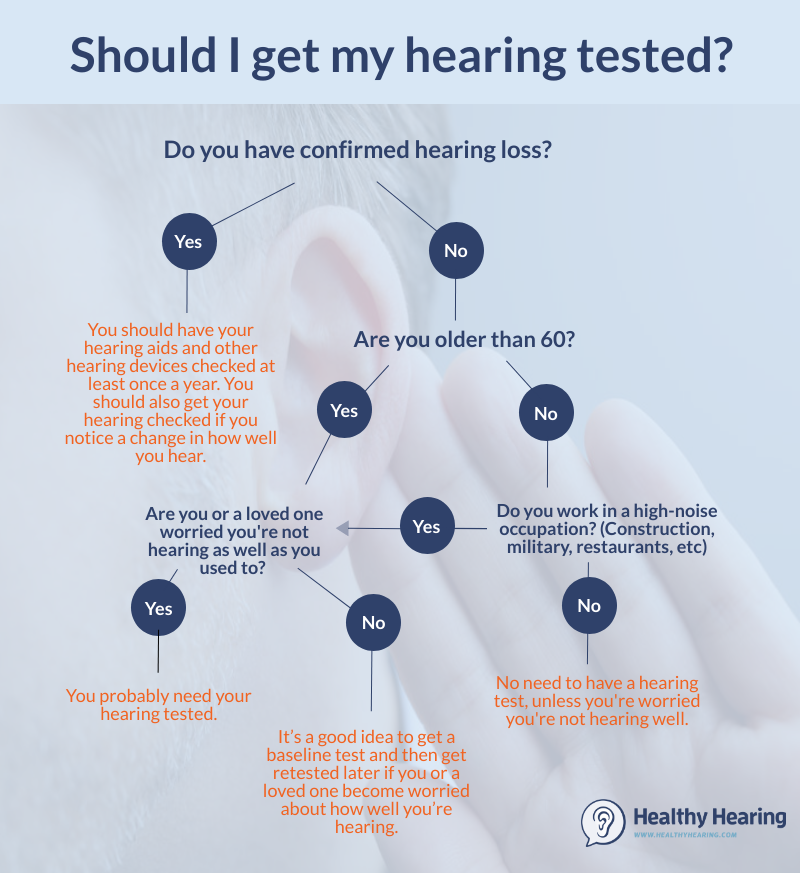 A hearing health historyWhen you visit the hearing clinic for the first time, office staff will have you fill out a case history form. This paperwork asks you a series of questions to help the hearing healthcare professional better understand your medical and hearing history and health. There are many potential causes of hearing loss, so the case history helps determine if you could have anything inherited or genetic in your family. Medical conditions like allergies, head colds, ear infections and even impacted earwax (cerumen) can also contribute to hearing loss. Also, the hearing health practitioner might ask if you’ve experienced any trauma to the head or ear structures. Any kind of injury to the cranial area can result in temporary or permanent hearing damage. Your hearing healthcare professional may also ask about your exposure to loud noises or if you work in a loud environment. Noise-induced hearing loss is very common in our sound-filled world. Finally, your hearing health professional might want to discuss the symptoms you are experiencing and how they are affecting your daily life. They will want to understand your lifestyle and the types of work, hobbies and social situations that are important to you. After your hearing health history is complete, the in-depth hearing test can begin. Getting a hearing test
Good news! Unlike a lot of medical tests, hearing tests are painless and non-invasive. Most occur in a quiet, sound-treated room (booth) or enclosure designed to keep out any other noises which might affect your hearing exam scores, such as the heater, air conditioner or office environment. You will be asked to wear headphones or soft earplugs with wires connected to an instrument called an audiometer that is used to conduct the test. The room may also be equipped with specially-placed speakers used for testing infants, small children or people who need to be tested while wearing hearing aids or cochlear implants. Pure-tone audiometryThis part of a hearing test usually involves pure-tone audiometry, which includes listening to tones at different pitches and volumes. It occurs in a sound-treated room. Your hearing care professional will communicate with you and provide instructions through your headphones. You will have to focus and listen carefully because you need to respond even if the tone sounds very soft and you can barely hear it. The test measures the very softest sounds you can hear at each frequency tested. Speech audiometrySpeech audiometry is another component of most hearing tests, and it uses recorded or live speech instead of pure tones, in a quiet setting. The speech portion of the exam evaluates the softest speech sounds (threshold) you can hear and understand. You will then be asked to repeat back words that are presented at a level well above threshold to see how well you can understand them accurately. Some practitioners use speech sounds to determine your most comfortable listening level and the upper limits of comfort for listening. Speech in noise and words in noise testsMost people complain about how they hear in noisy environments—not quiet sound-treated rooms, Common tests to replicate and quantify this hearing ability include the Connected Speech Test (CST), the Speech Perception in Noise test (SPIN), the Speech in Noise test (SIN or Quick SIN) and the Hearing in Noise Test (HINT). You may take one or more of these tests. During these tests you will listen to a speaker say words and statements while a soundtrack plays increasingly noisy sounds. These tests are useful for assessing “real-world” hearing ability, mimicking how you might hear in a restaurant or noisy grocery store. This information will help your hearing care professional understand what technology will work best for you. After you receive your hearing aids, you may take a similar test to fine-tune the amplification levels on your aid. Bone conduction testingIn some cases, a bone conduction test will also be given, which can help determine if the hearing loss is conductive or sensorineural. Treatment is generally different for people with conductive hearing loss. TympanometryIf necessary, the practitioner may perform tympanometry and a test of your acoustic reflexes. For these tests, a soft plug that creates pressure changes and generates sounds will be placed in the ear. This will determine how well your eardrum is moving and will measure the reflexive responses of the middle ear muscles. Testing for hidden hearing lossSome people have hearing loss that originates in their brain, and not their ears. This is known as hidden hearing loss. Standard hearing tests can't detect hidden hearing loss. If you passed your hearing test, but still feel like you can't hear well, you may have hidden hearing loss. Understanding your hearing test results
you. Test results are presented on a graph called an audiogram that displays the softest sounds you can hear at different pitches or frequencies. The vertical axis of an audiogram represents the intensity or volume of the sounds. The horizontal axis depicts the frequency or pitch of the sound. What an audiogram looks likeYour results will be plotted in decibels of hearing threshold level (dB HL). These units are unique to hearing testing but are based on the perception of sound pressure levels across all frequencies. For each tone you heard during the test, there will be a mark on the audiogram at the appropriate decibel level. Each ear is plotted separately and represented by two different lines. The lines may be quite similar and follow the same pattern or they may be very different. 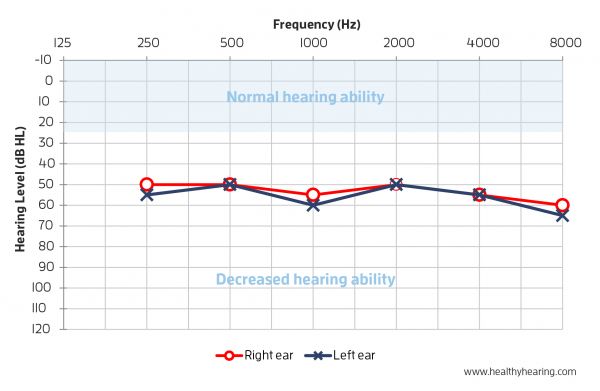 Degrees of hearing loss is measured in decibels (dB) and in the following categories:
Although some people talk about hearing loss in terms of percentage, it is not an appropriate or meaningful measure of hearing loss. It is very common to have more hearing loss at some frequencies than for others, so the percentage of hearing loss would be different at each test frequency, making it virtually meaningless when describing the overall hearing loss or determining a course of treatment. In a clinical setting, hearing loss is not described in percentages. However, it can be expressed in percentages for specific legal situations. In these cases decibels of hearing loss are converted using a recognized formula to create a "percentage of hearing loss" for legal purposes. Online hearing testsThere are a wide variety of hearing tests available online. Some are quiz-based screening tests (like ours), which can help you determine if you should go in for more rigorous in-person testing to determine the precise extent of your hearing loss. Some sites also have noise-based tests that let you listen to audio samples. Online hearing tests can provide people with a snapshot of their hearing status, but are by no means a replacement for a thorough diagnostic hearing evaluation. To find a trusted hearing care provider, our large directory of consumer-reviewed hearing clinics is a good place to start. Next steps after testingOnce your testing is complete, if you have hearing loss, your hearing care professional will recommend treatment. For most people with mild to moderate hearing loss, that means hearing aids. Fortunately, in recent years, hearing aids have become increasingly smaller and more advanced, often able to connect directly with smartphones and other devices. Talk to your hearing care provider about which options you should consider to help your hearing. Joy Victory, managing editor, Healthy Hearing
You are reading about: Related topics
More information about hearing aids, hearing aid brands, assistive devices and tinnitus. Featured clinics near me
Earzlink Hearing Care - Reynoldsburg Find a clinicWe have more hearing clinic reviews than any other site! Related contentThe Healthy Hearing Report |
|
www.HealthyHearing.com |
Hearing loss tests
By Joy Victory, managing editor, Healthy Hearing Last updated on: September 3rd, 2024 A thorough hearing test is easy and painless, and it will get you started on your path to better hearing. Find out what to expect when you are tested for hearing loss. |



 Joy Victory has extensive experience editing consumer health information. Her training in particular has focused on how to best communicate evidence-based medical guidelines and clinical trial results to the public. She strives to make health content accurate, accessible and engaging to the public.
Joy Victory has extensive experience editing consumer health information. Her training in particular has focused on how to best communicate evidence-based medical guidelines and clinical trial results to the public. She strives to make health content accurate, accessible and engaging to the public.