|
www.HealthyHearing.com |
All about: Over-the-counter hearing aidsOTC hearing aids can now be sold in stores and online
Contributed by Temma Ehrenfeld Are you thinking about buying hearing aids but not sure if over-the-counter is a good idea? It's understandable: There are many new OTC devices on the market, without a lot of information about their pros and cons. In October 2022, the FDA finalized their long-awaited OTC hearing aid guidance. The goal is to increase competition and ultimately make them more affordable, the FDA says. 
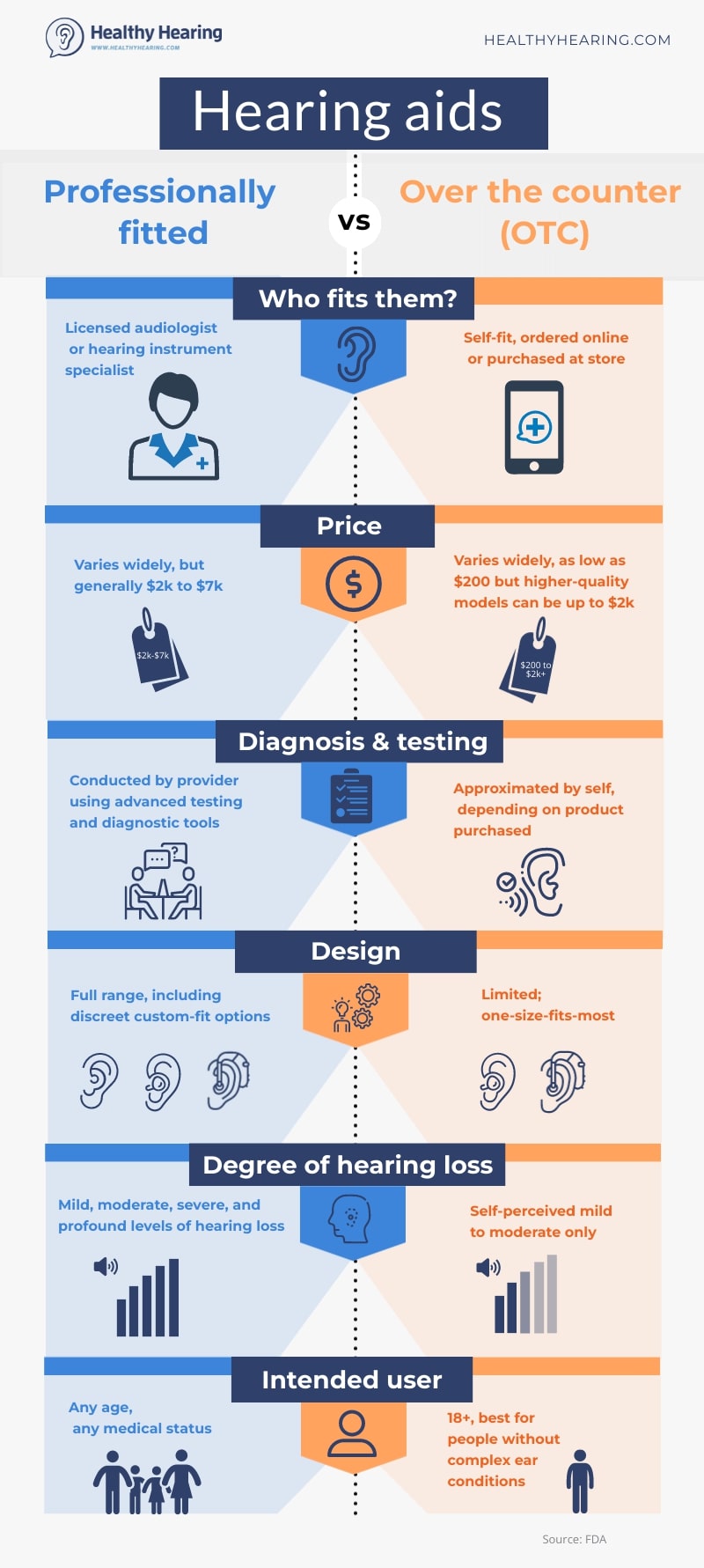
Perhaps the biggest change for consumers is that you no longer need to receive a hearing test or fitting by an audiologist or hearing professional to purchase hearing aids. However, anyone who has hearing loss can still see a hearing care professional for an in-person hearing test and fitting. Where do I get an OTC hearing aid?Over-the-counter hearing aids are available in pharmacies including CVS and Walgreens, some big box stores like Wal-Mart and Best Buy, as well as online. Traditional hearing aid clinics are also allowed to sell them, though they tend to specialize in devices with advanced hearing aid technology. Six key ways OTC hearing aids are different
OTC hearing aids are meant for adults who have a mild to moderate hearing loss, or for situational use like for use in a place of worship, restaurant or when watching TV. Pediatric hearing aids and hearing aids for severe to profound hearing loss will remain professionally-fitted devices, also called "prescription" hearing aids. Are they a good option for you?When it comes to programming OTC hearing aids for your unique type of hearing loss, virtually no face-to-face guidance is provided, which could be an issue for some people. “Since the user is on his or her own, people must be a bit tech-savvy,” says audiologist Juliëtte Sterkens, a consumer and hearing loop advocate for the Hearing Loss Association of America (HLAA). If updating your phone’s software system or downloading apps is easy for you, handling self-fitting hearing aids will generally be manageable. They also can be managed in the privacy of one’s home. That has some downsides, though. These devices come in a “one-size-fits-most ears" style, proper insertion of devices requires practice, and you're responsible for setting up the device, including the fitting and tuning of the sound and switching to the telecoil in public venues, Sterkens says. (Although so far, it doesn't seem like any OTC devices include telecoils, one of the core features found in the best hearing aids recommended by advocates.) And what about cost? So far, many of the models aren't that much cheaper than prescription hearing aids, either, especially the ones that allow more customization. "Even OTC hearing aids can cost a substantial amount, and consumers are advised to explore YouTube for videos that discuss features, and that show how to adjust and use the instruments," she recommends. How do I know if I have mild hearing loss?OTC hearing aids are limited in function compared to prescription hearing aids. If you have mild hearing loss and are holding back because of the cost of hearing aids, OTC hearing aids will be low-cost and will give you a taste of the advantages of better hearing. But what does "mild" look like in real life? You likely have mild or moderate hearing loss if:
Learn about these and other early warning signs of hearing loss. Who is not a good candidate for OTC?OTC hearing aids are not meant for everyone who has hearing loss. We recommend our in-depth piece on who should not get OTC hearing aids. If you have trouble hearing conversations even in quiet settings or miss loud sounds like cars honking when you drive or announcements in public buildings, your hearing loss is more severe than OTC hearing aids are designed to address, noted the National Institutes of Health. You need to see a doctor quickly if you have a sudden hearing loss, sudden plunge in your hearing (even if it improves), a big difference between one ear and the other, or tinnitus (ringing) in only one ear. These are possible signs of a medical problem. More: Will OTC hearing aids help with tinnitus? Things to consider when buying an OTC hearing aidThe HLAA recommends these questions to ask when buying an OTC hearing aid:
"Make sure to pay close attention to the return policy. In case OTC hearing aids don’t work out, you’ll want to know the process for returning them," recommends Michigan audiologist Amy Sarow. "Also, is there any person you can reach out to for support or questions? Some manufacturers have a phone number you can call or other options for support. It’s good to know your options in case you need them." And, be patient. "Getting used to hearing aids can take weeks, so be sure to give your brain the time to get used the amplification and hearing sounds differently," Sterkens says. What are my chances of being satisfied with an OTC hearing aid?A recent study showed that "premium" prescription hearing aids have the highest user satisfaction. This preference stemmed from factors related to comfort, specifically how the hearing aids processed background noise and how well the study participants could hear speech in a group setting. Because of the cost of the technology to develop these features, OTC hearing aids are unlikely to be as sophisticated. Input of knowledgeable provider is invaluableOther research indicates that people who've tried out OTC hearing aids greatly benefit from the help of a knowledgeable hearing care provider. This small 2017 trial provides some clues. It tested the outcome when adults aged 55 to 79 years with mild-to-moderate hearing loss chose among three pre-programmed hearing aids on their own for both ears. These were high-end digital mini-behind-the-ear aids, one of several common hearing aid styles. As Catherine Palmer, AuD, director of Audiology at the University of Pittsburgh, notes, a large majority—90 percent of participants—tried more than one hearing aid. But close to three-quarters picked the wrong aids based on their audiograms. In addition, although they saw a video and received handouts, 20 percent asked for extra help using the aids. The volunteers paid for their aids upfront and could get their money back if they chose to return their aids. The results: 55 percent wanted to keep them. More: Can my pharmacist help me with OTC hearing aids? Ongoing skilled hearing care is keyYour chances of satisfaction are higher if you receive a hearing aid fitted by a hearing instrument specialist or audiologist: In the study, a comparison group were fitted by audiologists and 81 percent of the volunteers wanted to keep their aids.
An additional wrinkle: The researchers gave everyone who didn’t want their aids a chance to work with an audiologist and wear the results over the next month. Of 10 people who had chosen among pre-programmed aids on their own who took that option, six did decide to keep their aids after working with an audiologist. 
you thorough testing to determine the extent of your hearing loss. This study suggests that for a better-than-even chance of satisfaction you will need the option to try different aids and help using your aids. Even so, your chances of getting hearing devices truly appropriate for your hearing loss are small, much lower than they would be if you work with an audiologist or hearing instrument specialist. More: What kind of specialist should I see for my hearing loss? A full-service hearing care provider can advise you about a variety of other devices that stream audio. If you have age-related vision loss, the choices are fairly simple: you can pick glasses and adjust the magnification and lighting on electronic devices. For hearing loss when you're older, there are many other options, including hearing aids, cochlear implants and assistive listening devices. Even where hearing aids are free, many people don't wear themPrice may not be the real reason you haven’t bought an aid. In Australia, Iceland and Germany public funding makes hearing aids free for many—yet many eligible people with significant hearing loss don’t wear hearing aids. When asked why they don’t wear hearing aids, people tend to say that the aids aren’t comfortable or didn’t give them natural hearing. (Note from author: As someone who has worn hearing aids for decades, I see those reasons as a sign you didn’t give hearing aids a chance. They aren’t comfortable–if you’re not used to them. There is an adjustment period. They also don’t give you “natural” hearing—but good natural hearing is beyond my reach. My choices are bad hearing or slightly artificial-sounding better hearing.) Those are all strong reasons to take action before your hearing declines further. If cost is truly the issue, OTC hearing aids could be an in-between step, or a life-changer, on your path to healthy hearing. What about very cheap hearing aids I'm finding online?If you've browsed online shopping sites, you've likely come across hearing aids that cost little more than a meal at a fancy restaurant. Be warned that these are likely not true hearing aids, but are "hearing amplifiers," also known as PSAPs, and they are not intended for use by people with hearing loss. Prefer specialized hearing care?Beyond helping you hear better, hearing aids are also linked to health benefits including reduced rates of depression and delayed onset of cognitive decline. The longer you wait, the harder it will be to treat your hearing loss. As many hearing providers say, "use it or lose it." If you're ready to take action, browse our directory of hearing aid clinics near you to make an appointment. Temma EhrenfeldTemma Ehrenfeld is an award-winning journalist who covers psychology and health. Her work has appeared in major newspapers, magazines and websites. You can find more of her writing at her Psychology Today blog, Open Gently. Read more about Temma.
Related Help Pages:
Hearing aids Bluetooth Fitting Prices Medicare Cleaning Accessories Cochlear implants Used hearing aids
|
Featured clinics near me
Earzlink Hearing Care - Reynoldsburg
7668 Slate Ridge Blvd
Reynoldsburg, OH 43068
HearingLife - Pickerington
10501 Blacklick Eastern Rd Suite 700
Pickerington, OH 43147


Find a clinic
Need a hearing test but not sure which clinic to choose?
Call 1-877-872-7165 for help setting up a hearing test appointment.